Meeting of the Board of Regents | May 2010
|
|
THE STATE EDUCATION DEPARTMENT / THE UNIVERSITY OF THE STATE OF NEW YORK / ALBANY, NY 12234 |
|
TO: |
|
|
FROM: |
|
|
SUBJECT: |
Standardization of Nursing Education for Licensure |
|
DATE: |
May 4, 2010 |
|
STRATEGIC GOAL: |
3 |
|
AUTHORIZATION(S): |
|
SUMMARY
Issue for Discussion
This item will provide the basis for a discussion of a legislative proposal to modify the educational requirements for registered professional nurses.
Reason(s) for Consideration
For information.
Proposed Handling
Presentation to the Professional Practice Committee.
Procedural History
On December 5, 2003, the New York State Board for Nursing unanimously approved a motion recommending that the Board of Regents and the Department consider support for a statutory or regulatory change permitting future registered nurse (RN) applicants who have completed an associate degree or diploma in nursing to continue to receive licensure as RNs but requiring such persons to obtain a baccalaureate degree in nursing within 10 years of initial licensure.
The proposal was adopted by the New York Organization of Nurse Executives (NYONE), an organization comprising the major employers of nurses throughout the state. NYONE has spearheaded this initiative, obtaining sponsors in both houses and developing bill language.
Background Information
Several research studies now demonstrate the added value of additional education in relation to patient outcomes. These studies show that increasing the number of baccalaureate nurses in an acute care hospital decreases the number of patient deaths.
The Nursing Board’s recommendation seeks to establish a uniform standard of education for licensure as a way of addressing quality patient care. In the current system, candidates who graduate from diploma, associate degree, or baccalaureate degree programs are all deemed qualified to take the identical licensure examination, are all licensed as RNs, and have identical workplace expectations. No other profession has such a wide range of educational levels to meet the same standard for licensure and practice. Moreover, because no demand is placed on nurses to pursue higher education, many do not. The Department’s 2002 Survey of Registered Nurses revealed that only 30% of the nurses prepared at the associate degree level have obtained an additional degree.
The proposed legislation would not eliminate any portion of the existing nursing workforce, nor does it require the closure of a single associate degree or diploma program. The recommendation is viewed by the Nursing Board as one that seeks to further expand the strengths of future associate degree and diploma prepared nurses to meet the ever increasingly complex health care needs of New York’s residents in the 21st Century.
Major provisions of the bills (S4051A; A2079B) include:
- Grandparenting of all currently licensed RNs to exempt them from ever having to meet the requirements of the bill;
- A four year lead-in time frame from the date of passage of the bill, to permit all students enrolled in associate or diploma programs to complete their studies and be grandparented and thus exempt from ever having to meet the bill’s requirements;
- Provisions that would place an RNs’ license on “hold” when the baccalaureate degree is not obtained in 10 years. This “hold” is similar to the action taken when a licensee fails to meet continuing education requirements in those professions that mandate continuing education as a criterion for continued registration;
- The opportunity for an extension beyond 10 years, for extenuating circumstances, as determined by the Department.
Given these provisions, if such a legislative proposal were passed by the legislature and signed by the Governor in 2010, no future license would be placed on “hold” until 2022.
This item is presented to provide information on this topic to the Professional Practice Committee and to seek the Committee’s guidance as the proposal is discussed and considered in the legislature. Additional information from the State Board for Nursing in support of its recommendation is contained in the attached document.
Attachment
MOVING TOWARD ADVANCED EDUCATION FOR NURSES
DIFFERENTIAL PATIENT OUTCOMES
Persuasive evidence validates the strong connection between nursing education levels and safe patient care. In September 2003, a landmark study on the educational levels of hospital nurses and surgical patient mortality was published in the Journal of the American Medical Association. The study examined outcomes data from 232,342 general, orthopedic and vascular surgery patients discharged from 168 (80%) of the 210 non-federal adult acute care general hospitals operating in Pennsylvania in 1999. The researchers, led by Dr. Linda Aiken from the University of Pennsylvania, found that patients experienced significantly lower mortality and failure to rescue rates (deaths among patients with complications) in hospitals where more baccalaureate prepared nurses provide direct patient care. The study found that rates of surgical patient deaths within 30 days of admission were 26 percent lower in hospitals with the highest proportion of baccalaureate prepared nurses. The research shows that a 10 percent increase in the proportion of nurses holding baccalaureate degrees in hospitals is directly related to a 5 percent decrease in the risk of patient deaths and failure to rescue. For example, as detailed in the chart below, in a hospital where the proportion of nurses with a baccalaureate or higher degree is 60 percent compared with one where it is 20 percent, there would be 14 fewer deaths from complications per 1,000 surgical patients. In addition, and not shown in the chart, there would be almost 4 fewer deaths per 1,000 surgical patients in general.
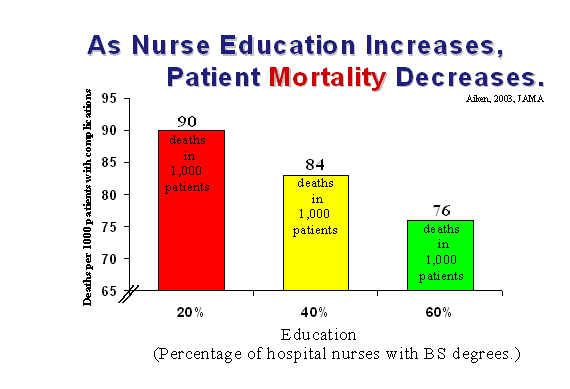
These findings were consistent after taking into consideration patient characteristics and hospital structural characteristics (size, teaching status, level of technology) as well as nurse staffing, nurse experience and whether the patient’s surgeon was board certified.
Years of experience did not independently predict mortality or failure to rescue. This study calls to question the notion that nurses’ years of experience are more influential on patient care than educational preparation.
Other findings of the Aiken study indicate that:
- Surgical patients cared for in hospitals with higher proportions of bed side RNs with bachelor’s degrees have a substantial survival advantage compared with those treated in hospitals with fewer staff nurses with BS degrees;
- Surgical patients with serious complications during hospitalization are significantly more likely to survive in hospitals with a higher proportion of RNs with BS degrees.
In May, 2008, Dr. Aiken released a study confirming her earlier findings which were published in the Journal of Nursing Administration.
In addition to Aiken’s research, several other studies also point to differences in nurses prepared at different educational levels.
- Dr. Carol Estabrooks replicated the Aiken study in 18,000 patients at 49 Canadian hospitals and found identical results which were published in the March/April 2005 issue of Nursing Research.
- In the January 2007 Journal of Advanced Nursing, Dr Ann Tourangeau published the results of a study of 46,993 patients and found hospitals with higher proportions of BS prepared nurses had lower rates of 30 day mortality. There were 9 fewer deaths per 1,000 discharges for every 10% increase in BS prepared nurses.
- In 2009, Drs. Mary Blegen and Colleen Goode completed a longitudinal study of 21 US hospitals over 84 quarters. The researchers found hospitals with a higher proportion of BSN educated nurses had lower rates of congestive heart failure mortality, hospital acquired pressure ulcers, failure to rescue, and length of inpatient stay. Their study has been submitted for publication.
CHANGES IN THE HEALTH CARE ENVIRONMENT
The National Advisory Council on Nurse Education and Practice, policy advisors to Congress and the U.S. Secretary of Health and Human Services on nursing issues, recommended in 2001 and again in 2009 that at least two-thirds of the nurse workforce hold baccalaureate or higher degrees in nursing by the year 2010. Their recommendation is based on the reality of significant changes in the environment in which RNs now practice brought about by major changes in drug therapy, equipment, rapid advances in technology, complex changes in health care delivery systems, increasing percentages of older adults with multiple chronic conditions, and expanding diversity of the country’s populace. Several examples follow:
- Half a century ago, intravenous therapy using very short needles was performed primarily by interns or physicians. In 2004, nurses thread long intravenous catheters from the elbow to the large veins lying very close to the heart so that all types of medications and fluid can be administered.
- Half a century ago intensive cardiac care units were experimental. In 2004, even rural hospitals have such units where nurses take responsibility for the hour-to-hour care of cardiac patients.
- In the 1960’s, nurses were responsible for knowing about approximately 600 prescription and over-the-counter drugs. In 2004, there are over 13,000 such commercial items. The pharmacy profession has responded by gradually increasing educational requirements for licensure starting with a BS degree in 1938, advancing to a 5-year BS degree in 1966 and most recently, in 2001, requiring a 6-year doctorate of pharmacy degree as the entry degree for licensure. Yet nurses remain responsible for knowing all of these drugs’ actions and untoward effects and teaching patients about them.
- In the 1960’s, computer literacy was an unknown term. In the 21st century, computer literacy will soon be an expected competence of nurses as they now begin to input notes and care plans and monitor patients’ laboratory values through computerized agency data files.
- In 1960, a typical surgical patient would remain in the hospital for 10 days. A new mother would stay for 5 days. Nurses took advantage of a lengthy preoperative time to prepare patients and their families for what to expect after surgery, to teach them ways to decrease postoperative complications, to establish a trusting relationship, and to assess the patients’ typical physical and mental state in order to be able to evaluate abnormalities and possible complications post-operatively. Today, nurses see many patients only as they exit the operating room still groggy from anesthesia. Nurses do not have baseline data about what the patient can see, hear or communicate under normal circumstances or what a normal blood pressure, breathing pattern or color is. Patients often have multiple surgical sites, multiple monitors, artificial respirators and medications that knock out normal respirations, leaving the patient completely dependent, and several intravenous lines with potentially lethal medications if the rate of infusion is not correct. Hospitals have turned into intensive care units with an average length of stay of 2.9 days. These workforce changes require a more educated practicing nurse with higher levels of professional knowledge and judgment and an expanded set of clinical and management skills.
Not only must today’s RN have the knowledge to monitor patients’ health status, perform therapeutic treatments, and provide expert care and patient education within a constricted time frame, but today’s RN must also be able to practice as a peer in interdisciplinary teams and integrate evidence-based clinical knowledge and research with knowledge of culturally diverse communities and their resources.
By 2020, persons from groups currently termed “minority” will be in the majority. Nurses will need to have additional courses in sociology, anthropology, and ethics to provide effective nursing care to such diverse populations. That education cannot easily be provided in an associate degree or diploma program where curricula are already packed with essential nursing education courses and basic science courses such as anatomy, physiology, chemistry, and biology. In addition, diploma and associate degree nursing programs generally focus, as they should, on the care of acute hospitalized patients. The curricula of RN to BS programs focus on community and public health, where, increasingly, health care needs are rising as patients are rapidly discharged from hospitals to receive continuing nursing care within their communities.
The evolution of the health care environment is recognized by other health care providers as evidenced by the following:
- In the 1950s, both occupational therapists (OTs) and physical therapists (PTs) could be certified without a college degree. At present, a bachelor’s degree is required for licensure as a physical therapist, and the national accrediting organization for physical therapy programs only recognizes master’s degree programs; it is expected that, by 2020, a doctoral degree will be expected. Similarly, a bachelor’s degree is now required for licensure as an occupational therapist and only post-baccalaureate occupational therapy programs are being accredited by the national accrediting body.
- Since their recognition as regulated professions in the early 1980s practitioners of speech-language pathology and audiology have needed a master’s degree for licensure.
- As of September 2004, a master’s degree is required for new licensure as a licensed master’s social worker or licensed clinical social worker.
- A baccalaureate degree or higher is required for licensure as an athletic trainer.
A comparison of select professions regulated by the Office of the Professions is presented in the chart below.
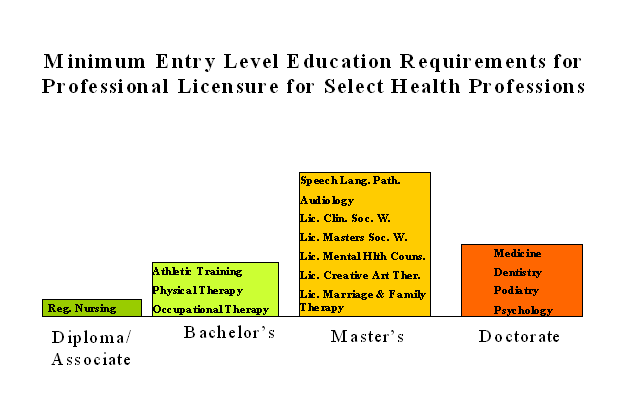
THE ROLE OF THE HEALTH CARE TEAM IN PATIENT CARE
In 2001, the Institute of Medicine (IOM) report, Crossing the Quality Chasm: A New Health System for the 21st Century, provided numerous study findings documenting estimates as high as 98,000 annually for the number of hospitalized Americans dying each year as a result of errors in their care—more than those who die from motor vehicle accidents, breast cancer or AIDS. The report recommended follow-up by an interdisciplinary summit that would develop next steps for reform of health professions education. The IOM’s 2003 report on Health Professions Education: A Bridge to Quality is one response to that recommendation. The report identified the need for all health-related educational programs and institutions to share a vision to educate health professionals to deliver patient-centered care as members of an interdisciplinary team emphasizing evidence-based practice, quality improvement approaches, and informatics. Physicians in the American College of Critical Care Medicine are on record that, “Critical care nurses do the majority of patient assessment, evaluation and care in the intensive care unit,” while a study of medication errors in two hospitals over a 6-month time frame found that nurses were responsible for preventing 86 percent of all medication errors made by physicians, pharmacists and others involved in providing medications for patients. Because nurses are the health care providers patients are most likely to encounter and with whom patients spend the greatest amount of time, nurses are uniquely positioned to rescue patients from impending or actual complications and prevent fragmentation of care. To accomplish this goal however, advanced education is needed in order for nurses to have similar skills in negotiation, systems theory, change theory, and research as their partners from other disciplines within such an interdisciplinary team.
Registered nurses are primarily responsible for direct patient care and on-going care coordination. To be effective members of the interdisciplinary health care team advocated by the IOM, it is important that nurses complete the necessary education to prepare them to fulfill their pivotal professional roles.
NURSING EDUCATION IN OTHER COUNTRIES
According to a 2002 book published by the World Bank titled, Constructing Knowledge Societies: New Challenges for Tertiary Education, knowledge has become the single most important factor in economic development and global competitiveness. Thus, it is no small surprise that other nations have responded to the demand for nurses with greater knowledge by requiring a baccalaureate degree for any individual seeking licensure as an RN. In several countries, education obtained in a diploma or associate degree nursing program is no longer accepted for professional nursing licensure as multiple educational pathways into nursing have been eliminated in preference for the baccalaureate degree. Such countries include Australia, New Zealand, Philippines, Ireland, Iceland, Cuba and all members of the European Union. In Canada, most provinces limit licensure as an RN to individuals prepared at the baccalaureate level. January 1, 2005 marked the date when the Province of Ontario began to limit RN licensure to baccalaureate prepared individuals despite a nursing shortage greater than that experienced in the United States. The Canadian Nurses Association persuaded Canadian governmental agencies, health care facilities, nurses, and the general public to demand the broad-based bachelor’s degree as a requirement for nursing licensure based on new RN practice competencies for today’s health care system. None of the provinces have found that this position has decreased the number of students applying to nursing programs; in fact, interest in nursing has increased as reflected in the increase in nursing applications to baccalaureate nursing programs.
STRATEGIES TO FACILITATE NURSES’ SECURING HIGHER EDUCATION
Based on meetings with deans and faculty of New York State nursing programs and information from nursing programs throughout the country, it is the position of the State Board for Nursing that sufficient educational programs exist to provide the education needed by future associate degree or diploma prepared nurses to obtain a baccalaureate degree within 10 years of initial licensure. At a meeting of the Council of Deans of Nursing, Senior Colleges and Universities of New York State, deans and faculty unanimously agreed that their capacity to educate RNs seeking baccalaureate degrees was significant and that their programs could accept the increases proposed by the Nursing Board’s recommendation.
Each of the 55 New York State institutions providing Department-registered nursing programs leading to the baccalaureate degree offers programs that make special accommodations for associate degree or diploma prepared RNs seeking to advance their education. Twenty-nine institutions offer 32 registered nursing programs specifically structured for RNs seeking to complete the baccalaureate degree.
Several examples follow that demonstrate efforts by programs to encourage RN students to pursue baccalaureate degree study.
- In addition to articulation agreements with 11 different universities and colleges, Queensborough Community College’s Department of Nursing is also in partnership with Hunter Bellevue School of Nursing to increase the number of baccalaureate prepared nurses at the bedside. The project partners these two programs with dual enrollment and innovative curriculum that promote seamless student transition into baccalaureate programs. The curricula will increase content in gerontological and public health nursing and will creatively utilize technological learning strategies to prepare a nurse for the current health care environment. It is anticipated that this model will provide a template for other partnerships within the City University of New York. In fact, CUNY’s Lehman College has begun dialogue with Hostos Community College, LaGuardia Community College and Bronx Community College for just such an endeavor.
- A unique dual degree partnership has also been begun between St. Joseph’s College of Nursing, which prepares nurses with an associate’s degree in Nursing and Le Moyne College, which confers the baccalaureate degree. Students apply to and must be accepted full-time into both of the nursing programs. They spend the first year taking core college courses at LeMoyne College. The second and third years at St. Joseph’s College of Nursing emphasize hands-on patient care. At the conclusion of the third year they may take the national licensing exam to become an RN and then complete their baccalaureate degree back at LeMoyne College in the fourth year. This model has also been adopted by Daemen College in collaboration with Erie Community College, Niagara County Community College and Trocaire College, as well as SUNY Institute of Technology in collaboration with St. Elizabeth’s College of Nursing in Utica.
- Pace University’s Lienhard School of Nursing has 12 articulation agreements with associate degree nursing programs to facilitate entry, progression and graduation from their RN to BS program.
- Mercy College’s Nursing Program has developed numerous articulation agreements with associate degree nursing programs and offers a high quality baccalaureate degree that grants appropriate credit and builds on past learning.
- D’Youville College added a “completion” program for graduates of nursing diploma programs in 1957. A more flexible program is currently in place to provide a high quality completion program for associate degree nursing graduates with several articulation agreements to facilitate ease of transferring credits.
- Hartwick College began offering a Registered Nurse Mobility program in the mid-1980s. In 2001, the College began a partnership program with Bassett Healthcare, SUNY Delhi and other two-year colleges to provide RNs a baccalaureate degree in nursing that includes a discounted tuition rate, recognizes all of the lower division nursing work for study at the associate degree level and is offered in a two-day format allowing nurses to continue to work full-time while completing all required course work.
- The University of Rochester School of Nursing has articulation agreements with several nearby community colleges in an effort to provide a seamless curriculum for students interested in pursuing the baccalaureate degree in nursing. More recently, the school offers 32 nursing credits for RNs from any accredited non-baccalaureate nursing program wishing to advance to the BS degree.
- SUNY Plattsburgh has developed a state-of-the-art delivery system that offers a distance learning baccalaureate completion program for associate degree and diploma prepared RNs. Classes are offered on-site at the Adirondack, Jefferson, Cayuga and Fulton-Montgomery community colleges and at the Alice Hyde Medical Center in Malone.
- Nursing faculty at Keuka College, Long Island University-Brooklyn Campus and others have contracted with health care facilities, some local, some at considerable distance from the college/university, to provide nursing coursework at hospitals to groups of RN employees seeking to advance to the baccalaureate degree.
- SUNY Stony Brook offers a totally on-line RN to BS completion program, which requires no commuting, or career interruption.
- The Dean of Excelsior College’s School of Nursing stated in a March 2004 letter that “We have enhanced the articulation between diploma and associate degree programs with our baccalaureate program [and] have unlimited capacity to respond to student demand.”
Accelerated baccalaureate programs for students with baccalaureate degrees in other disciplines is a rather new phenomenon, which has potential for adding new individuals to the nursing workforce. These programs allow students with a baccalaureate degree, but without nursing experience, to earn a nursing degree in less time (between 11 months to 2 years for most programs). Such programs enable nursing schools to produce more baccalaureate degree-nursing graduates over a shorter period of time while attracting new talent that might not otherwise have considered nursing as a career. Of the 53 accelerated-baccalaureate nursing programs that exist nationwide, 14 are located in New York State.
Distance education, which is made possible by new technologies not available in the 1960s, is another promising means of educating RNs who seek to obtain their baccalaureate degree. Internet-based nursing programs have grown rapidly in recent years, and New York students and nursing programs are taking advantage of these new technologies.
- In 2004, SUNY at Stony Brook began its completely on-line RN to BS nursing program.
- Maria College in Albany has established an articulation agreement with Drexel University in Philadelphia for acceptance of Maria’s associate degree prepared students into Drexel’s on-line RN-BS completion program.
- Seton Hall University in New Jersey offers an on-line RN to BS program with only three weekends required on site to meet the residency requirement.
Nursing education leaders throughout New York have joined to develop a unified articulation plan that would ease the transition from associate degree to baccalaureate degree education. The plan guarantees 30 nursing credits to graduates of New York State associate degree programs seeking to continue their education at the baccalaureate level. In addition to advanced placement for nursing courses completed at the associate degree level, students would also receive credit for successfully completed liberal arts, science, and humanities courses. Administrators and faculty from the Associate Degree Nursing Council and the Council of Deans of Nursing, Senior Colleges and Universities of New York State have collaborated regionally to assure the adoption of this plan.
CONCLUSION
In the past, many initiatives for solving the diversity of educational levels in nursing have been proposed. Each of these proposals either eliminated diploma and associate degree programs or reduced them to a lower level of practice. All of the proposals met with substantial resistance from a variety of factions in nursing. The Nursing Board’s recommendation is uniquely different in that it does not require the end of diploma or associate degree education. Rather, it recognizes the diploma and associate degree in nursing as important entry points for many into the profession; that diploma and associate degree nursing education are academically demanding and clinically challenging courses of study; and that the abilities of diploma and associate degree nursing graduates are demonstrated in high NCLEX pass rates and excellent feedback from employers. The recommendation also recognizes that additional education makes a difference in the skill and competence of nurses, just as it does for other health professionals. By maintaining diploma and associate degree entry, the Nursing Board’s recommendation provides a reasonable compromise in lieu of many of the more radical plans for standardization being proposed by other countries, states, and agencies. Given the enhancements to articulation between associate and baccalaureate nursing programs and the ever-increasing options for advanced placement and distance learning, the proposal can be implemented without disadvantaging future new graduates. Nurses require a strong knowledge base in liberal arts and sciences as well as advanced clinical, analytical and interpersonal skills in order to practice safely in the increasingly complex, highly technological, and culturally diverse health care community. By advancing to the baccalaureate degree the Board’s motion seeks to be responsive to meet the increasingly complex health care needs of the residents of New York State.





